Teaching Family Medicine and General Practice
Article information
Abstract
The teaching of family medicine and general practice should aim to develop an appreciation of the unique nature and role of the specialty. Teachers should relate patient cases to the principles of family medicine. These principles include (1) compassionate care; (2) a generalist/holistic approach focusing on the whole person, family, and community; (3) continuity of relationship, i.e., building a patient-physician bond of trust; (4) reflective mindfulness; and (5) lifelong learning. The curriculum, instructional strategy, and assessment should be carefully aligned. Core competencies include patient-centered communication, physical examination skills, clinical procedures, palliative care, humanities in medicine, holistic care, shared decision-making, family therapy, home and community visits, chronic disease care, problem-based documentation, team-based care, data-driven improvement, information mastery, ethics and professionalism, and work-life balance. Family medicine/general practice is defined as the medical specialty that manages common and long-term illnesses, focusing on overall health and well-being. Hence, clerkship schedules should maximize clinical exposure and opportunities for self-reflection. A learner-centered approach should begin with a self-identified inventory of learning needs based on the curriculum; next, these needs should be chosen as topics for student presentations. Teaching methods should include mini-workshops: a combination of didactic lectures and small-group exercises. Individual face-to-face formative feedback should occur at midcourse and culminate in a group reflection on the learning experience. Clinical supervision should gradually decrease as each resident demonstrates safe patient care. Procedure skills training should be closely supervised, formally documented, and constitute about one-fourth of learning sessions.
INTRODUCTION
This article aims to provide a practical framework for teaching family medicine and general practice. The target audience includes family physicians/general practitioners (GPs) (as faculty or clinic preceptors), course coordinators, and other teaching staff involved in family medicine education. Family medicine is taught at medical colleges to medical students in clerkships ranging from 4 weeks to 3 months to a longitudinal experience spanning the entire training. At the postgraduate level, a 2- to 4-year training program for residents/registrars permits eligibility to sit for a family medicine specialty board examination. Family medicine as a career option is also available to nurse practitioners and physician assistants in certain countries.
To provide evidence-based recommendations, we searched PubMed MEDLINE with the keywords “teaching family medicine general practice” using the “best match” sort order. The “similar articles” feature was used to find additional articles. The search was limited to English language references, humans, articles with an abstract, original research, and date of publication within the last 10 years. Inclusion criteria included randomized controlled trials (with or without blinding) of teaching methods and well-designed cohort studies with concurrent control groups. Exclusion criteria were lack of objectively measured learning outcomes or the effect of educational intervention on patient outcomes. The search yielded 263 articles, nine of which met the criteria for valid, reliable, and reproducible research. Despite the dearth of studies meeting these criteria, there exists a rich literature on family medicine education based on expert opinion and subjective outcomes, such as learner satisfaction. Additional recommendations are based on the author’s experience of teaching family medicine for over 2 decades in North America and Asia. The following is an integrative review of the best practices in teaching and learning family medicine.
1. The Aim of Teaching Family Medicine and General Practice
The primary and overriding aim of teaching family medicine and general practice to medical students is to develop an appreciation for the unique and vital role of the specialty within the healthcare system. This is an affective learning goal, as opposed to a knowledge-based cognitive outcome. Thus, it requires committed, passionate teachers who can foster reflection and inspire learners. Clinician-teacher role models who understand the ethos of family medicine are needed in practice settings. A well-planned family medicine clerkship can have a positive influence on career choice among medical students [1].
At the postgraduate level, training should be geared toward independent, unsupervised clinical practice. This requires building strong clinical competencies for common illnesses seen in primary care. Mastery learning is the goal of family medicine residency training. Thus, the duration of training should be extended for residents/registrars who are assessed as pre-competent. It is not enough for a resident to display a positive attitude toward learning; faculty-observed achievement of core competencies must be documented. The underlying themes, principles, and philosophies of family medicine should be woven into the entire length of the training program.
2. Terms Defined
Family medicine/general practice is defined as the medical specialty that manages common and long-term illnesses, focusing on overall health and well-being [2]. As a clinical specialty, it is at par with internal medicine, pediatrics, and surgery and should not be associated or linked to non-clinical fields, such as community medicine and public health. While many family physicians engage in community health and social activism, their primary activity is direct patient care.
The two terms, “family medicine” and “general practice,” are synonymous and can be used interchangeably. Trained specialists in this field are called family physicians or GPs. In some parts of the world, a medical college graduate who practices primary care without further training is also referred to as a GP, in a somewhat deprecatory manner. Therefore, the term family physician is preferred for those with postgraduate training in the specialty. The obsolete terms “family practice” and “family practitioner” should not be used. Similarly, pejorative terms such as “gatekeeper” and “primary care provider” should be avoided, as primary care is a health system component, and not the name of a clinical specialty. Apart from family physicians, general internists (also called general physicians in some regions) and general pediatricians also provide primary care. These terms should be clarified to medical students.
Misconceptions about general practice should be addressed but not dwelt upon excessively. It may be helpful for students to think of family medicine as a clinical specialty with its own body of knowledge, research, and philosophy. The scope of general practice does not cover comprehensive care for all medical diseases. This incredible claim is a source of confusion and disillusionment for medical students and lay public. It discredits GPs as being incompetent and perpetuates the myth that to be a GP, one must know medicine, pediatrics, and obstetrics and gynecology along with orthopedics, dermatology, and other fields. Common illnesses are the scope of family medicine. These include common acute and chronic diseases that are prevalent in the community. Thus, the scope varies to some extent from region to region. Osteoarthritis, peptic ulcers, asthma, infections, and skin problems are common in most communities, but in some parts of the world, HIV/AIDS (human immunodeficiency virus/acquired immunodeficiency syndrome) and tuberculosis are familiar to family physicians. In other regions, GPs manage diabetes, heart disease, end-of-life care, obstetrics, sports medicine, and psychiatric illnesses as part of their routine day-to-day work. Family physicians perform a wide range of clinical procedures. These includes skin surgery, non-operative orthopedics, many obstetric and gynecologic procedures (that are performed in a clinic), cosmetic and laser treatments, as well as administering infusions such as biologic therapies. Therefore, a minimum of one-fourth of the teaching sessions should be dedicated to hands-on procedure skills training (the “one-fourth rule”). Clinical privileges, the permission to perform these procedures by family physicians, must be assertively defended at administrative meetings in hospitals. In summary, the scope of general practice consists of common diseases with some regional variations. This has direct implications for curriculum content.
COURSE CONTENT
1. Clerkship Curriculum
At the undergraduate level, the curriculum is aimed at inculcating the principles of family medicine and general practice (Table 1) [3]. These abstract concepts are taught through patient cases seen in the clinic. While these cases will include details of medical management, such as choosing drugs and tests, the underlying goal is to appreciate the role of family physicians in healthcare. By focusing on the principles, students can link concepts, such as continuity and mindfulness, to better patient outcomes. When moderating case discussions, faculty should regularly refer to specific terms such as holistic approach, family dynamics, culture, continuity, access, and patient-centered care. Hence, it does not suffice to simply place medical students in GP clinics and end the rotation with a supervisor evaluation form. Family medicine faculty should conduct training seminars for community GPs.
Clinical topics for the clerkship should be chosen from common illnesses prevalent in the region [4]. An appropriate mix of presenting common symptoms, acute illnesses, chronic diseases, and clinical procedures should be covered (Table 2). The responsibility for teaching clinical topics depends on the length of the clerkship, number of students per group, and the size of the family medicine department. Larger family medicine departments can take on a greater number of clinical topics. Topics in clinical medicine must be equitably shared between family medicine, internal medicine, pediatrics, and other clinical specialties. Family medicine clerkships should focus on higher-order concepts rather than attempting to cover a large number of diseases.
2. Residency Curriculum
At the postgraduate level, a more explicit curriculum with predefined competencies is needed (Table 1). These competencies, listed in the rightmost column of Table 1, should be mastered by the end of the training. Residents are more likely to remain on track if these expectations are communicated clearly and reinforced repeatedly. At the postgraduate level, competencies are fairly complex and multidimensional [5-7]. However, complicated curriculum schemes with dozens of broad competencies tend be impractical [8]. Broadly speaking, core competencies can be categorized into three domains: patient care (including communication skills, medical knowledge and procedures), practice management (including systems-based improvement), and lifelong learning (Table 1). A narrow focus on medical knowledge can be detrimental to the development of a resident’s higher-order skills.
While residency education is driven by competence in patient care and clinical procedures, certain higher-order skills are the hallmarks of family physicians. These include patient-centered care, evidence-based medicine and information mastery, palliative care and family counseling [9]. New competencies have arisen recently such as genomic medicine, multi-morbidity, aging, and cancer as a chronic illness [10]. Medical informatics, or more broadly health informatics, drives modern medicine. Tomorrow’s physicians need to be savvy with technology as well as adaptive to changing regulatory and reimbursement environments [11,12].
INSTRUCTIONAL DESIGN
1. Course Structure
For medical students, a minimum of 8 weeks is recommended for family medicine/general practice clerkships in the final clinical year. A few students will require additional weeks for remedial learning. This duration is recommended based on the experiential time needed to build continuity of care and allow students to manage patients at follow-up visits. Given its primary importance, other subspecialty rotations should be condensed to accommodate family medicine [13]. Early exposure of first year medical students to clinical medicine should not be delegated solely to general practice [14]. Due to its high-level holistic approach to clinical reasoning and patient care, family medicine is suited for the senior year of medical college. Longitudinal integrated clerkships appear to be equivalent to block rotations [15]. Medical students’ exposure to other subspecialties should be prohibited and non-family medicine projects such as laboratory research must be forbidden during the clerkship.
Postgraduate residents or registrars must complete at least 2 years of supervised training. Some trainees will require additional years. All residents must provide continuity of care to an assigned panel of patient families in a longitudinal weekly clinic. This clinic should be increased from once a week in the first year to up to 4 times a week in the final year. The goal is mastery learning. Thus, the faculty should not permit registrars to graduate until they can demonstrate and document a high standard of clinical competence.
2. Orientation Session
All new groups should start with an orientation session (also called induction). In this session, faculty members and students introduce themselves, perhaps sharing personal backgrounds and thoughts, such as what inspired them to pursue medicine as a career. In this setting, discussing specialty choices or persuading students to choose general practice is not recommended. Moreover, students’ preconceived (sometimes negative and stereotypical) notions about general practice should not be elicited. The atmosphere and tone of the discussion should be warm and welcoming. A positive and enthusiastic faculty attitude on the first day can create an impression that lasts the entire program. Course coordinators should avoid threatening comments or overemphasis on disciplinary actions for unprofessional conduct. Students should be shown the layout of the clinic and introduced to the staff on a first-name basis. Some practical guidance on “dos and don’ts” may be helpful, as well as clear and detailed instructions on practical aspects, such as clinic timings and assessment methods. On the orientation day, a survey of personal learning needs should be conducted.
3. Learning Needs Assessment
In this questionnaire, students rate their “level of comfort” for each item in a list of family medicine topics (Table 2). Each student should develop a personal learning plan based on his/her self-identified needs. Ratings should be averaged, and topics that are most needed should be selected for student (or faculty) presentations. All family medicine faculty members and clinic preceptors should review the results to gauge the learning needs of the group.
An alternative to self-reported learning needs is a formative assessment, such as an examination covering a wide range of curriculum topics. A practice test on the first day of the course might appear counterintuitive but is a useful tool for understanding the learning needs of the medical students.
4. Learning Plan and Log Book or Portfolio
A personal learning plan enables students and residents to play an active role in their professional development. Students can identify their reading priorities using a learning needs questionnaire. The learning plan should also be used in one-to-one discussions with the faculty to track progress. This discussion may lead to individualized activities, such as student presentations, elective placements, and research projects. The learning plan should be placed in a logbook. The logbook or portfolio, either print or electronic, is a record of patient cases, procedures, reflective writing, assessment report cards, feedback from faculty, clinical placements, and student presentations [16]. A reading log should be encouraged. Experiential learning in which students are engaged in community projects enables students to understand practical issues faced by patients [17]. During patient care, learners should write down clinical queries in their logbooks for searching online later on [18]. Advanced activities such as quality improvement projects, research studies, multidisciplinary case discussions, grand rounds, and home visits should be documented as part of the learning journey.
5. Active Learning
Medical students and residents should be encouraged to become active learners. Active learners are self-directed, proactively seek feedback, and take responsibility for their professional development. The faculty should foster self-directed learning in their interactions with students. This can be achieved by discussing learning goals and plans. Students should be asked to fill out a learning plan template that should be reviewed periodically. Learners should be provided training on online resources. Instead of arbitrary assignments, encouraging students and residents to reflect on patient care can foster active learning. Finally, eliciting feedback on whether the student’s questions were answered and if the supervisor was satisfactory may be helpful. This approach to supporting active learner engagement is superior to traditional placement at clinical sites, culminating in a final exit examination [19].
6. Clinical Teaching
The primary teaching method in family medicine remains patient-based. It can occur in any setting, such as ambulatory clinics (also called office or surgery), hospitals, nursing homes, and home visits. Clinical patient care should be maximized (over classroom sessions) when planning student schedules, as it correlates with learning [20]. Students and residents must be observed when performing medical interviews, physical examinations, and clinical procedures. A frequent shortcoming of clinical training is the lack of direct observation by supervising physicians.
Supervising family physicians, whether faculty or community preceptors, should be trained on how to teach during patient care [21]. This includes asking facilitating questions, involving students in patient care and sharing clinical expertise [22]. For experienced teachers, the presence of students does not increase patient visit time [23].
Community preceptors should be guided on how to adapt teaching intensity based on patient waiting times. During busy periods, students may need to assume the role of observers and help guide patients to different clinical areas. Alternatively, students may interview patients in a separate room and then present the case to the supervising physician in a precepting room. Both strategies are equally satisfactory to patients and students [24]. Clinical supervision of residents should be titrated carefully. As these physicians-in-training show increasing clinical competence, the need to observe and discuss each case decreases, a process referred to as entrustment [25,26]. Patient safety and medical errors are major concerns with decreased direct supervision, and systems must be in place for blameless disclosure and open door access to senior faculty members. Residents should be encouraged to become patient advocates by visiting community health services and conducting home visits [27]. A mission-driven approach to community health and prevention requires awareness of social determinants of health, such as health literacy and access to care.
Continuity of relationships should be ensured by constructing clinical teams and assigning families of patients to each team, a process known as empanelment.
To support teaching and learning, a few modifications to the clinic are helpful. A teaching room should be equipped with a round table and chairs, a whiteboard, reference books (especially family medicine textbooks and atlases), and an internet-connected computer with a projector and a printer. Additionally, patient education materials, clinical decision charts, disease-specific patient questionnaires, plastic anatomic models, and medical instruments are useful. Faculty members can remain in this room, while residents and medical students drop in to discuss cases as needed. The room can be used for small-group discussions, including student presentations.
7. Teaching Skills
Teaching clinical medicine requires expertise and tact. Great teachers are great communicators. They are keen observers and listeners who are able to recognize teachable moments. During discussions, clinic preceptors can use specific micro-skills to enhance learning. Examples include asking for supportive findings for a diagnosis, teaching general rules, reinforcing and correcting clinical thinking, and identifying learning needs [28]. Supervisors should avoid asking rote recall questions, such as a list of causes for a clinical finding. Differential diagnoses can be grouped into probable, unlikely, and serious. Specific and objective feedback should be offered tactfully and in privacy. Residents should be encouraged to have medical students with them during clinics, after receiving training on teaching. Learning progress, such as clinical queries discussed, should be documented in a logbook or a portfolio.
8. Academic Day
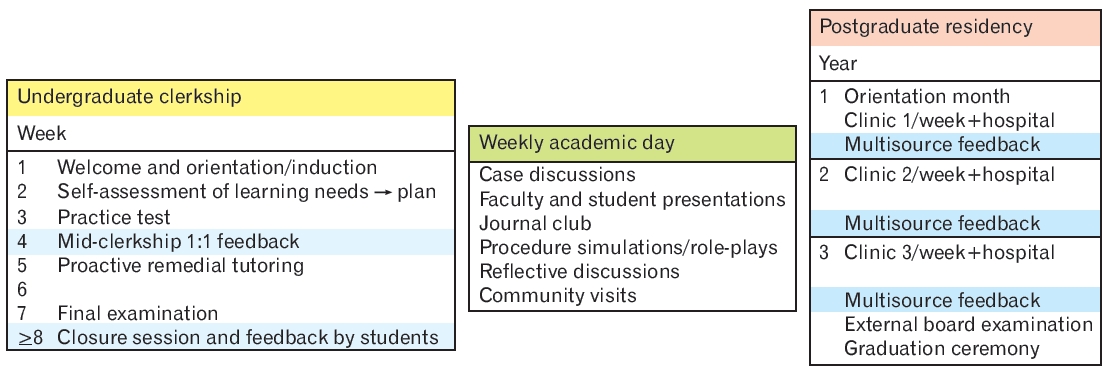
Typically, one day of the week is reserved for classroom teaching—the academic day (Figure 1). This enables medical students (in family medicine clerkships) and postgraduate registrars/residents placed in different clinics to come together for interactive learning and group bonding. Recommended activities for the academic day include patient case discussions, journal clubs (preferably from family medicine journals), role-plays for communication skills, procedure skills simulations, visual diagnosis using clinical images, multiple-choice questions in a group setting using an audience response system, clinical videos, research project planning, group reflection on difficult issues, invited talks, and community outreach activities. Invited speakers should preferentially be family physicians [29]. A faculty member or a senior resident, who must be informed about the clinical details in advance, should moderate case discussions to allow everyone to participate equally. An alternative to the relatively ineffective traditional journal club is a discussion based on clinical questions that arise during patient care, the “Clinical Query.” Such discussions focus on real clinical needs and lead to more meaningful, patient-oriented learning. Clinical procedures can be taught efficiently using video modules rather than a traditional lecture-demonstration [30]. Group discussion sessions on improving self-efficacy can lead to resilience and reduced perceived stress among residents [31]. Sources of stress among GP trainees include knowledge/uncertainty, workload and portfolios [32]. Humanities and arts in medicine should be discussed, touching on the human experience of illness and suffering.
A limited role remains for teacher-directed traditional approaches, such as topic-based didactic lectures and family medicine textbooks. These structured teaching strategies may provide a scaffold for students at early stages of learning. A combination of formal didactic lectures with small-group discussions is more effective than either one alone [33]. The mini-workshop is a new teaching format that combines a didactic lecture with small-group exercises [34]. In the first 20 minutes, a faculty member delivers a non-interactive lecture that includes definitions, clinical approach, common errors, and illustrative cases. This is followed by small-group problem-solving exercises for 40 minutes or more. The teacher distributes case-based short-answer questions to each group and then walks around to assist any group that needs help. To facilitate discussion, it is preferable to have three students per group. For closure, the suggested answers to each question are displayed at the end of the session. The mini-workshop enables building foundation knowledge as well as active learner participation in a structured format.
9. Blended Learning
The combination of face-to-face teaching with online learning is termed blended learning. Family medicine residents seem to learn equally well with face-to-face presentations, web-based modules, and live presentations, followed by role-plays [35].
Online learning management systems have features such as discussion forums, quizzes, and structured lessons with text and videos. Students placed at different clinics can exchange ideas and “clinical pearls” online. Blogs allow the posting of cases (without identifying details) and reflective writing for discussion via comments. This can foster reflection and mindfulness during patient care. Remarkably, higher-order concepts such as cross-cultural communication can be taught using online modules [36].
10. Placement at Distant Clinics
When placing students at distant sites, such as rural clinics, course coordinators should support clinic preceptors with training and feedback. This should include teaching tips, online resources, and telephone discussions about student performance. Preceptors should be recognized for their contribution with remuneration, continuing professional development certificates, adjunct faculty appointments, and access to the learning management system. Students and residents at these sites should write a brief reflective report at the end of the placement.
ASSESSMENT
1. Practice Tests
Family medicine clerkships should conduct a mid-clerkship practice test. More frequent testing is recommended for residency programs. These formative assessments should be formally proctored but not count towards the final marks. The report card should include a graph showing breakdown of performance based on curriculum topics or organ systems. The faculty can use the results to guide students in one-to-one discussions while reviewing individual learning plans.
2. Clinical Skills Assessment
Clinical skills such as medical interviewing, physical examination, and procedure skills must be assessed in a structured format in the clinic as well as in a simulation center. These assessments should be well planned in advance, as they require substantial effort and administrative coordination to implement [37]. Structured checklists need to be developed and reviewed. Each item in the checklist should be a directly observable behavior, such as “sanitized hands before touching the patient.” Items should start with a verb, such as observed, palpated, or asked. A clinical logbook is not a substitute for directly observed assessments. A debriefing session after the examination, in which students receive group feedback on their overall performance, is essential. The use of real patients is not necessary, as plastic manikin models suffice. The long case and oral interviews (viva voce) are now considered too subjective in medical education. Since complex psychomotor skills are being assessed, the checklists and other examination details can be disclosed to students prior to the examination session.
One structured format for protecting examination integrity and ensuring fairness is competency evaluation using randomized testing [38]. In this format, the skills stations are modified slightly from student to student so that some of the correct responses are different. For example, a chest X-ray interpretation station changes from emphysema to pneumonia to heart failure. While the skill tested remains the same, scores must be adjusted to compensate for the difficulty of each variant.
3. Clinical Knowledge Assessment
A working foundation for medical knowledge is necessary for the safe practice of medicine. Even with the availability of point-of-care clinical decision support tools such as online resources, apps, and electronic health records, physicians need knowledge and expertise to provide care in real time. Objectively marked assessments, such as single-best answer multiple-choice questions (MCQs), are widely used. Despite the dissatisfaction voiced by some clinicians, MCQs are a reliable and valid measure of clinical knowledge application. With a reasonably large number of questions, an MCQ-based examination is superior to an oral interview or essay in discriminating between competent and pre-competent learners. More significantly, MCQs can assess the application of knowledge and not merely recall facts. This requires careful construction of MCQs based on brief patient scenarios with laboratory results and clinical images. MCQs may be adapted from existing banks instead of writing de novo. Questions should cover the full scope of general practice, a process known as curriculum-assessment mapping or “blueprinting.” Thus, common emergencies, obstetric care, sports medicine, and geriatrics need to be represented. Questions, or items, as they are sometimes called, should reflect the nature of general practice. That is, clinical severity should be variable (with normal variants), common diseases should be more frequent as question items as well as correct answers, and the core principles should be prominent. When assessing abstract concepts such as ethics, professionalism, and the principles of family medicine, the answer options should be physician actions or counseling expressions, instead of names of principles.
4. Work-Based Assessment
Subjective evaluations by supervisors are a mandatory part of professional training. However, this originates more from traditional and stakeholder preferences than from educational research. The chief advantage is the direct observation by a supervisor in a practice setting. Other benefits include enforcing student attendance and participation in clinical care, supporting experiential learning, and guiding learners toward desirable behaviors. The evaluation form should include domains such as patient-centered communication skills, physical examination, clinical reasoning, lifelong learning, and professionalism. The form can include a rubric detailing desirable behaviors such as punctuality, dress code, and teamwork. Feedback from non-physician staff, such as nurses and medical assistants, can contribute to a multisource “360” assessment. Work-based assessments should be discussed with residents. This discussion should include self-reflection by residents and written updates in the learning plan.
CONCLUSION
Teaching family medicine is an art guided by educational research. Desirable qualities of clinical teachers include exceptional listening skills, keen observation of clinical details, a discerning perception of patients’ needs, an ability to foresee a patient’s clinical course, ease with clinical uncertainty, community activism, and value based (cost conscious) care. The clerkship and residency should be well-organized and thoughtfully designed. Friendly and caring teachers can enhance learner satisfaction. Overall, family physicians should embody the joy of building relationships with patients and their families, sharing moments of sorrow and recovery, and making a difference in the lives of people.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
Acknowledgements
The author would like to acknowledge the contributions made by teachers of family medicine and general practice worldwide.