|
 |
- Search
| Korean J Fam Med > Volume 35(5); 2014 > Article |
Abstract
Background
The objective of this study was to investigate the relationship between smoking and metabolic syndrome in men.
Methods
This cross-sectional study included 1,852 men over age 40 who underwent health screening from April 2009 to December 2010. We classified them into three smoking levels as non-, intermediate-, and heavy-smoker, considering their smoking status (non, ex, current) and amount (0, 1-29, Ōēź30 pack year [PYR]). The relationship between smoking level and metabolic syndrome was analyzed by logistic regression analysis, after covariates (age, body mass index, education, house income, alcohol intake, and physical activity) were controlled.
Results
The proportions of non-, intermediate-, and heavy-smokers were 31.8%, 56.2%, and 12.0%, respectively. Odds ratios (ORs) and 95% confidence intervals (95% CIs) for metabolic syndrome were 1.0, 1.58 (1.09-2.23), 1.92 (1.29-2.81) in non-, intermediate-, and heavy-smokers, respectively. For heavy-smokers compared with non-smokers, ORs and 95% CIs of a lower high density lipoprotein cholesterol, higher triglyceride, and higher fasting glucose were 2.47 (1.63-3.74), 1.71 (1.17-2.52), and 1.43 (1.02-2.00), respectively. In current-smokers, we divided into three subgroups according to PYR, and compared with 1-19 PYR, ORs and 95% CIs of 20-29 PYR and Ōēź30 PYR for metabolic syndrome were 2.07 (1.14-3.74) and 3.06 (1.66-5.62), respectively.
For prevention and management of chronic diseases, improvement of health behaviors such as smoking, drinking, diet, and physical activity are most effective.1) Smoking, known as the worst health behavior, is not only a risk factor that causes cardiovascular disease and malignant tumor,2,3) but is also related to metabolic disease such as diabetes and obesity,4) and even passive smoking is damaging to health.5) It has been demonstrated that smoking is associated with reduced insulin sensitivity and diabetes risk,6) impaired lipid metabolism,7) abdominal obesity by abdominal fat accumulation,8) increased blood pressure,9) oxidative stress, and artherosclerosis.10)
Metabolic syndrome (MS), a surrogate indicator of type 2 diabetes and cardiovascular disease, refers to a group of disease conditions including abdominal obesity, dyslipidemia, high blood pressure, and insulin resistance.11) As mentioned above, most metabolic effects of smoking are overlapped with (those of) MS. For these reasons, it has been increasing interest that the relationship between smoking and cardiovascular was mediated by MS.12)
Although a few studies suggested that smoking may have a preventive effect on MS,13,14) but recently it turns out to be a false result caused by the confounder effect of obesity, the preventive effect of smoking was disappeared after weight was controlled.15) As a result, smoking is an independent risk factor for MS and showed a dose-response relationship with MS.16) Long-term smoking causes insulin resistance and increase the risk of MS and diabetes, regardless of current or past smoking.5,17)
Smoking level has two components: one is 'smoking status,' referring to non-smoking, ex-smoking, and current-smoking and the other is 'smoking amount,' referring to non-smoking, intermediate-smoking, and heavy-smoking according to pack year (PYR: "how many years did you smoke about 1 pack per day?"; the concept of whole-life smoking amount). However, there are limitations in this oversimplified classification; smoking status is likely to underestimate past-smoking or overestimate current-smoking, and smoking amount also ignores time effect on human body because low-grade inflammation, such as MS, is able to recover by effective intervention.
Therefore, in this cross-sectional study, we divided study participants into three groups according to smoking level as non-(never smoking), heavy-(current smoking and Ōēź30 PYR), and intermediate-smoker (other), considering smoking status and smoking amount, then we investigated the relationship between smoking and MS.
One thousand nine hundred and sixty men over age 40 who underwent health examination from April 2009 to December 2010 agreed to sign the informed-consent for this study. One hundred and eight persons were excluded if they had the target disease of MS (myocardial infarction, angina, stroke, and diabetes; n = 74) or incomplete answers (n = 34). As a result, a total of 1,852 persons were included.
Demographic and lifestyle data were collected by a trained interviewer using a questionnaire, and anthropometric and blood test were conducted concurrently.
Reliable and persuasive estimates are required to assess smoking level. Two aspects of smoking were considered, 'smoking status' (non-, ex-, current smoking) and 'smoking amount' (PYR: average daily smoking amount [pack] ├Ś smoking period [year]; 0 PYR, 1-29 PYR, and Ōēź30 PYR). We classified study participants into three groups as non-(never smoking), heavy-(current smoking and Ōēź30 PYR), and intermediate-smokers (other) according to smoking level.
For the definition of MS, the criteria of the modified National Cholesterol Education Program Adult Treatment Panel III (2007)18) were followed when more than three of the five conditions were met: (1) waist circumference Ōēź90 cm; (2) blood pressure Ōēź130/85 mm Hg or medication; (3) triglyceride Ōēź150 mg/dL or medication; (4) fasting glucose Ōēź100 mg/dL or medication; (5) high density lipoprotein (HDL) cholesterol <40 mg/dL.
Education was divided into nine levels: no education, withdrawn from elementary school, elementary graduate or withdrawn from middle school, middle school graduated or withdrawn from high school, high school graduate, college graduate, withdrawn from university, university graduate, and graduate school. House income (monthly) was divided into eight levels: <0.5, 0.5-1.0, 1.0-1.5, 1.5-2.0, 2.0-3.0, 3.0-4.0, 4.0-6.0, and Ōēź6.0 million won.
Smoking, drinking, and leisure time physical activities of study participants were examined. As for drinking, kinds of alcohol were listed including soju, beer, makgulli, sake, wine, whisky, champaign, and others. And average daily alcohol consumption for the last year was calculated by monthly drinking frequency and average amount of one drink. Using the Korean version of the Minnesoita Leisura-Time Physical Activity Questionnaire (MLTPAQ),19) energy expenditure (kcal/d) was calculated as the metabolic equivalent of task that is unique for each physical activity during leisure time.
Height and weight were measured in a standing position to obtain body mass index (BMI, kg/m2). Waist circumference was measured at the level of the iliac crest in a standing position. Systolic blood pressure and diastolic blood pressure were measured after relaxing for more than 5 minutes, and the average values were obtained after repeated measurements. As for blood testing, the blood samples were collected from the brachial vein after fasting for at least 8 hours, and fasting blood glucose, triglyceride, total cholesterol, HDL cholesterol, high-sensitivity C-reactive protein (hs-CRP), and gamma-glutamyltransferase (GGT) were measured.
IBM SPSS ver. 19.0 (IBM Co., Armonk, NY, USA) were used for data analysis and a P-value <0.05 was regarded as significant. Logistic regression was performed to obtain odds ratios (ORs) and 95% confidence intervals (95% CIs) of smoking with MS, after adjusting for age, BMI, education, house income, alcohol amounts (g/d), and physical activity (kcal/d) as covariates. Chi-square tests and analysis of variance were conducted to compare education, house income, drinking, physical activity, BMI, blood test results, and MS with smoking level. The participants who already had hypertension medication (285 persons) were considered to have hypertension components of MS regardless of measured value. We excluded 285 persons after the relationship of smoking and high blood pressure was analyzed.
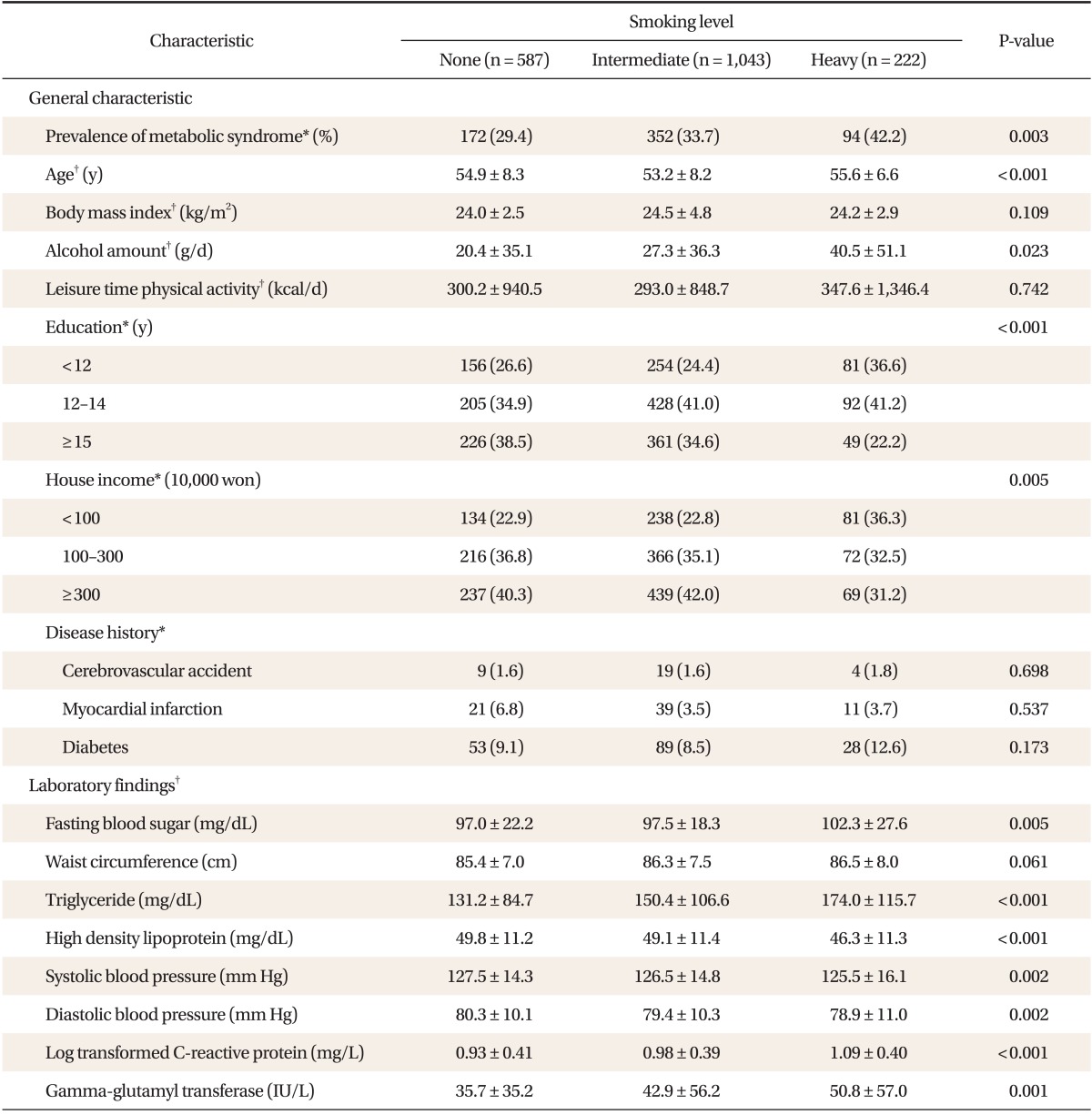
Of the 1,852 subjects, the proportions of non-, intermediate-, and heavy-smoker were 31.8% (587 persons), 56.2% (1,043 persons), and 12.0% (222 persons), respectively and the prevalence of MS were 29.4%, 33.7%, and 42.2%, respectively. The prevalence of MS was increased as smoking level increased. Education and house income level was inversely associated with smoking level, and daily alcohol consumption increased with smoking level, but physical activity was not significant. Fasting glucose, triglyceride, and HDL were worse, but blood pressure improved as smoking increased, hs-CRP (log transformed) and GGT, which reflect low-level inflammation, increased as smoking increased (Table 1).
Smoking showed a positive relationship with components of MS. After adjusting for covariates (age, BMI, alcohol amounts, daily physical activity, education, house income), OR was set as 1 in non-smoker, and odds ratios (ORs) and 95% confidence intervals (95% CIs) of intermediate- and heavy-smokers for fasting glucose were 1.11 (0.81-1.51), 1.43 (1.02-2.00), for triglyceride 1.47 (1.03-2.11), 1.71 (1.17-2.52), and for HDL 2.07 (1.41-3.02), 2.47 (1.63-3.74) (Table 2).
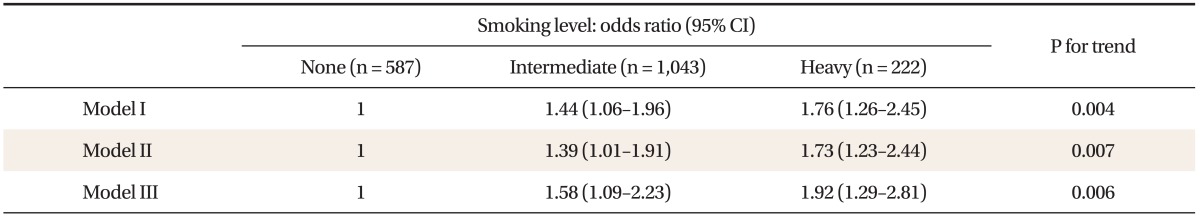
OR was set as 1 in non-smokers without adjusting for covariates, and ORs and 95% CIs for MS in intermediate- and heavy-smokers were 1.44 (1.06-1.96) and 1.76 (1.26-2.45) (model I). After age and BMI was adjusted, ORs and 95% CIs in intermediate- and heavy-smokers were 1.39 (1.01-1.91) and 1.73 (1.23-2.44) (model II). After age, BMI, education, house income, alcohol amounts (g/d), and physical activity (kcal/d) were adjusted for, ORs and 95% CIs in intermediate- and heavy-smokers were 1.58 (1.09-2.23) and 1.92 (1.29-2.81) (model III). Thus, the prevalence of MS linearly increased as smoking level increased (Table 3).
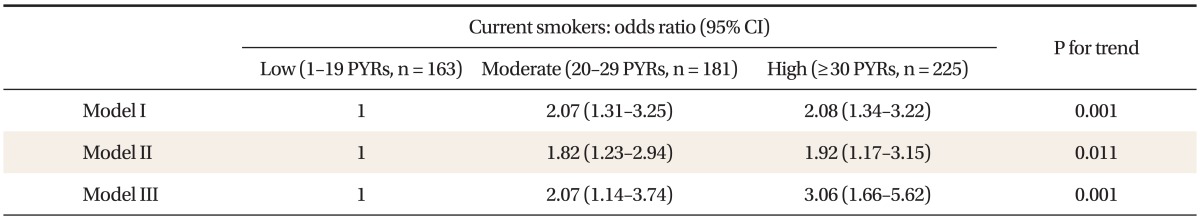
Among participants, proportions of non-, ex-, and current-smoking were 29.3% (542 persons), 40.0% (741 persons), and 30.7% (569 persons), respectively. After non-, and ex-smokers were excluded, we divided current-smokers into three subgroups according to PYR (1-19 PYR; 20-29 PYR; Ōēź30 PYR), and compared the prevalence of MS. When OR was set as 1 in the 1-19 PYR, after adjusting for covariates (age, BMI, alcohol amounts, physical activity, education, and house income), ORs and 95% CIs in 20-29 PYR and Ōēź30 PYR were 2.07 (1.14-3.74) and 3.06 (1.66-5.62), respectively (Table 4).
In this study, the risk of MS showed a dose-response relationship ORs 1.58 and 1.92 in intermediate- and heavy-smokers compared with non-smokers. These results were consistent with other domestic and foreign studies.14,20) In Korea National Health and Nutrition Examination Survey (KNHANES, 1998), ORs and 95% CIs were 1.2 (0.9-1.6), 1.5 (1.2-2.1), and 1.6 (1.1-2.1) in ex-, intermediate-, and heavy-smokers, respectively, compared with that of non-smokers.16) In another three-year follow-up domestic study, relative risk and 95% Cis were 1.90 (1.21-3.00) in current smoker (Ōēź1 pack/d) and 1.66 (1.18-2.33) in long term smoker, compared with non-smoker.15) In a Japanese study conducted on white-collar workers, ORs and 95% CIs were 1.30 (1.00-1.68), 1.17 (0.88-1.56), and 1.66 (1.24-2.20) in ex-, intermediate-, and heavy-smokers, compared with non-smokers.18) This cross-sectional study showed that hs-CRP20) and GGT,21) which are low-level inflammation markers, also linearly increased with smoking level.
Biologically, the most important factor in the relationship between smoking and MS is insulin resistance caused by complicated reactions of cotinine, carbon mono oxide (CO), cortisol, the sympathetic nervous system, and growth hormone. Cotinine, a metabolite of nicotine, induces a low-level inflammation response,22) and nicotine, CO, cortisol, the sympathetic nervous system, and growth hormone activate anti-estrogen effects and finally reduce insulin sensitivity.19,23)
In addition, socioeconomic factors such as education and income, and lifestyle factors such as drinking and physical activity were closely correlated with the incidence of metabolic syndrome.24,25) Their results were consistent with ours.
Among components of MS, HDL, triglyceride, and glucose were associated with smoking level, and our results were consistent with those of other studies showing that smoking decreases HDL, increases LDL, and increases insulin resistance.7,26) In previous experimental studies and prospective studies, smoking increased arterial hardness and blood pressure,10,27,28) and promoted visceral fat accumulation,29) thereby worsening abdominal obesity related diseases.30,31)
However, There was no significant relationship among smoking, blood pressure, and abdominal obesity in this study. We considered limitations of a cross-sectional study that could explain the difference. In addition, there were controversies over the relationship between smoking and blood pressure.20,27,31)
The limitations of this study are as follows. First, this study was conducted in a health promotion center of single university hospital. Thus, generalization of the results is impossible. However, compared to KNHANES (1998), the participants of this study were older, more educated, and smoked less (in KNHNES, Ōēź20 years, proportion of over high school graduate was 27.2% and proportion of heavy smoker was 16.3%; in this study, Ōēź40 years, over high school was 38.5% and heavy smoker was 12.0%). We could infer null effects between age and education for smoking level that attenuated selection bias. Second, as a cross-sectional study, it could not explain the causality between smoking and MS. Third, information and recall bias caused by willful and illusory memory could not be excluded.
Despite the limitations, one strength of this study is that the smoking assessment had multiple components, including both smoking status and amount, and the relationship between smoking and MS was analyzed after controlling various variables.
References
1. Woolf SH, Jonas S, Kaplan-Liss E. Health promotion and disease prevention in clinical practice. 2nd ed. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2008.
2. Hong Y, Pedersen NL, Brismar K, de Faire U. Genetic and environmental architecture of the features of the insulin-resistance syndrome. Am J Hum Genet 1997;60:143-152. PMID: 8981957.


3. Kim MH, Kim MK, Choi BY, Shin YJ. Prevalence of the metabolic syndrome and its association with cardiovascular diseases in Korea. J Korean Med Sci 2004;19:195-201. PMID: 15082890.



4. Chiolero A, Faeh D, Paccaud F, Cornuz J. Consequences of smoking for body weight, body fat distribution, and insulin resistance. Am J Clin Nutr 2008;87:801-809. PMID: 18400700.


5. Hong AR, Lee KS, Lee SY, Yu JH. Association of current and past smoking with metabolic syndrome in men. J Prev Med Public Health 2009;42:160-164. PMID: 19491558.


6. Bergman BC, Perreault L, Hunerdosse D, Kerege A, Playdon M, Samek AM, et al. Novel and reversible mechanisms of smoking-induced insulin resistance in humans. Diabetes 2012;61:3156-3166. PMID: 22966072.



7. Anazawa T, Dimayuga PC, Li H, Tani S, Bradfield J, Chyu KY, et al. Effect of exposure to cigarette smoke on carotid artery intimal thickening: the role of inducible NO synthase. Arterioscler Thromb Vasc Biol 2004;24:1652-1658. PMID: 15271786.


8. Despres JP, Lemieux I. Abdominal obesity and metabolic syndrome. Nature 2006;444:881-887. PMID: 17167477.


9. Orth SR. Effects of smoking on systemic and intrarenal hemodynamics: influence on renal function. J Am Soc Nephrol 2004;15(Suppl 1):S58-S63. PMID: 14684675.


10. Pasupathi P, Rao YY, Farook J, Saravanan G, Bakthavathsalam G. Effect of cigarette smoking on lipids and oxidative stress biomarkers in patients with acute myocardial infarction. Res J Med Med Sci 2009;4:151-159.
11. Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA, et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 2005;112:2735-2752. PMID: 16157765.


12. Dzien A, Dzien-Bischinger C, Hoppichler F, Lechleitner M. The metabolic syndrome as a link between smoking and cardiovascular disease. Diabetes Obes Metab 2004;6:127-132. PMID: 14746578.


13. Onat A, Ozhan H, Esen AM, Albayrak S, Karabulut A, Can G, et al. Prospective epidemiologic evidence of a "protective" effect of smoking on metabolic syndrome and diabetes among Turkish women: without associated overall health benefit. Atherosclerosis 2007;193:380-388. PMID: 16926017.


14. Cena H, Fonte ML, Turconi G. Relationship between smoking and metabolic syndrome. Nutr Rev 2011;69:745-753. PMID: 22133198.


15. Kim BJ, Kim BS, Sung KC, Kang JH, Lee MH, Park JR. Association of smoking status, weight change, and incident metabolic syndrome in men: a 3-year follow-up study. Diabetes Care 2009;32:1314-1316. PMID: 19389815.


16. Park HS, Oh SW, Kang JH, Park YW, Choi JM, Kim YS, et al. Prevalence and associated factors with metabolic syndrome in South Korea: from the Korean National Health and Nutrition Examination Survey, 1998. J Korean Soc Study Obes 2003;12:1-14.
17. Targher G, Alberiche M, Zenere MB, Bonadonna RC, Muggeo M, Bonora E. Cigarette smoking and insulin resistance in patients with noninsulin-dependent diabetes mellitus. J Clin Endocrinol Metab 1997;82:3619-3624. PMID: 9360516.


18. Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA, et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 2005;112:2735-2752. PMID: 16157765.


19. Kim DH. Effect of job and leisure time physical activity on the risk of colorectal cancer: a case-control study [dissertation]. Seoul: Seoul National University; 1997.
20. Lee HY, Kim JS, Kang SH, Yoo JH. Association between smoking status, C-reactive protein and the metabolic syndrome in long-term smokers among middle-aged Korean men. J Korean Acad Fam Med 2008;29:94-101.
21. Lee DH, Blomhoff R, Jacobs DR Jr. Is serum gamma glutamyltransferase a marker of oxidative stress? Free Radic Res 2004;38:535-539. PMID: 15346644.


22. Cryer PE, Haymond MW, Santiago JV, Shah SD. Norepinephrine and epinephrine release and adrenergic mediation of smoking-associated hemodynamic and metabolic events. N Engl J Med 1976;295:573-577. PMID: 950972.


23. Weitzman M, Cook S, Auinger P, Florin TA, Daniels S, Nguyen M, et al. Tobacco smoke exposure is associated with the metabolic syndrome in adolescents. Circulation 2005;112:862-869. PMID: 16061737.


24. Slater C, Carlton B. Behavior, lifestyle, and socioeconomic variables as determinants of health status: implications for health policy development. Am J Prev Med 1985;1:25-33. PMID: 3916715.

25. Yamamoto A, Temba H, Horibe H, Mabuchi H, Saito Y, Matsuzawa Y, et al. Life style and cardiovascular risk factors in the Japanese population: from an epidemiological survey on serum lipid levels in Japan 1990 part 1: influence of life style and excess body weight on HDL cholesterol and other lipid parameters in men. J Atheroscler Thromb 2003;10:165-175. PMID: 14564086.


26. Rhee MY, Na SH, Kim YK, Lee MM, Kim HY. Acute effects of cigarette smoking on arterial stiffness and blood pressure in male smokers with hypertension. Am J Hypertens 2007;20:637-641. PMID: 17531920.


27. Mizuno O, Okamoto K, Sawada M, Mimura M, Watanabe T, Morishita T. Obesity and smoking: relationship with waist circumference and obesity-related disorders in men undergoing a health screening. J Atheroscler Thromb 2005;12:199-204. PMID: 16141623.


28. Virdis A, Giannarelli C, Neves MF, Taddei S, Ghiadoni L. Cigarette smoking and hypertension. Curr Pharm Des 2010;16:2518-2525. PMID: 20550499.


29. DeFina LF, Vega GL, Leonard D, Grundy SM. Fasting glucose, obesity, and metabolic syndrome as predictors of type 2 diabetes: the Cooper Center Longitudinal Study. J Investig Med 2012;60:1164-1168.


30. Katzmarzyk PT, Janssen I, Ross R, Church TS, Blair SN. The importance of waist circumference in the definition of metabolic syndrome: prospective analyses of mortality in men. Diabetes Care 2006;29:404-409. PMID: 16443895.


31. Ishizaka N, Ishizaka Y, Toda E, Hashimoto H, Nagai R, Yamakado M. Association between cigarette smoking, metabolic syndrome, and carotid arteriosclerosis in Japanese individuals. Atherosclerosis 2005;181:381-388. PMID: 16039294.


Table┬Ā2
Odds ratios (95% confidence interval) of MS components according to smoking status by multiple logistic regression

Table┬Ā3
Odds ratio (95% CI) of metabolic syndrome according to smoking level by multiple logistic regression
- TOOLS